I know, there are many things to worry about in the world, and this is low on the list. I do get frustrated when I see RD publications giving the same party line about the risks of a Paleo diet and not mentioning the growing group of studies actually examining the relative pros/cons of the diet. For the record, I know the staff has a commitment to good work and quality writing. I think this story missed the mark in terms of providing a balanced view of the current research.
If there’s a belief that there’s a value in seeing a nutrition professional, because nutrition is about facts, not beliefs, professionals should be talking about the data and not opinions, right? Even and especially when it doesn’t line up with what we learned in school.
I know grains are the bottom of the food guide pyramid, or plate. Citing data on whole grains vs refined actually isn’t relevant to the question of the relative merits of grain-free diet and how that may differ by disease state. It actually fully misses the point.
From my perspective the data is interesting and encouraging, but it also isn’t a slam dunk. I’d rather see bigger studies and ones that are better controlled. I went into some of the weaknesses in the early literature in a prior post.
FWIW, I’m not a Paleo advocate per se. I am a research advocate. 😉 It seems like Paleo advocates say there are mountains of research (nope) while others suggest there’s no study, which isn’t true, either. I have mixed feelings about Paleo and think there are pros and cons–and more importantly, pros and cons giving a given person’s needs, medical history and lifestyle. Generally, I am more interested in what is on someone’s plate than what trendy label is attached to it.
I think the newest study on autoimmune Paleo and IBD is fascinating, and so is the MS research and the rest of the studies below. And it does seem that a Paleo diet has helped people safely lose weight and improve CVD risk factors, which is what counts at the end of the day.
Because I’m short on time, I’m only including research here through 2016, which is the last time I did a thorough lit review. Detailed references are below the charts. I don’t have time right now to update for 2017-18
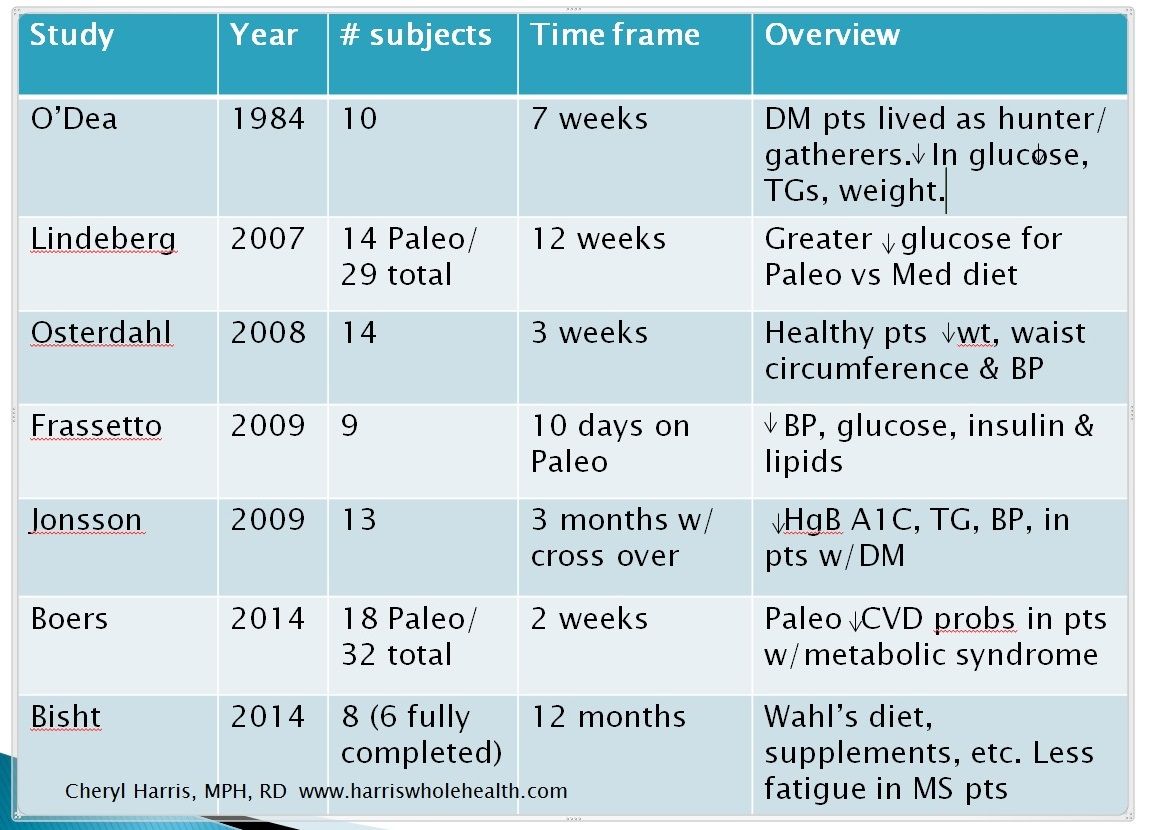
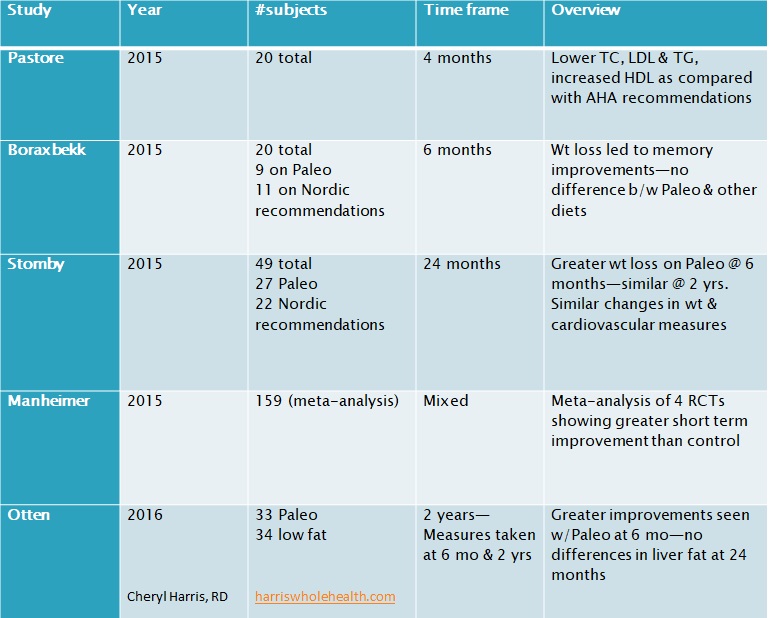 Frassetto LA, Schloetter M, Mietus-Synder M, Morris RC, Jr., Sebastian A: Metabolic and physiologic improvements from consuming a paleolithic, hunter-gatherer type diet. Eur J Clin Nutr 2009.
Frassetto LA, Schloetter M, Mietus-Synder M, Morris RC, Jr., Sebastian A: Metabolic and physiologic improvements from consuming a paleolithic, hunter-gatherer type diet. Eur J Clin Nutr 2009.
Jönsson T, Granfeldt Y, Ahrén B, Branell UC, Pålsson G, Hansson A, Söderström M, Lindeberg S. Beneficial effects of a Paleolithic diet on cardiovascular risk factors in type 2 diabetes: a randomized cross-over pilot study. Cardiovasc Diabetol. 2009;8:35
Lindeberg S, Jonsson T, Granfeldt Y, Borgstrand E, Soffman J, Sjostrom K, Ahren B: A Palaeolithic diet improves glucose tolerance more than a Mediterranean-like diet in individuals with ischaemic heart disease. Diabetologia 2007, 50(9):1795-1807.
O’Dea K: Marked improvement in carbohydrate and lipid metabolism in diabetic Australian aborigines after temporary reversion to traditional lifestyle. Diabetes 1984, 33(6):596-603.
Osterdahl M, Kocturk T, Koochek A, Wandell PE: Effects of a short-term intervention with a paleolithic diet in healthy volunteers. Eur J Clin Nutr 2008, 62(5):682-685.
Boers I, Muskiet FA, Berkelaar E, Schut E. et al. Favourable effects of consuming a Palaeolithic-type diet on characteristics of the metabolic syndrome: a randomized controlled pilot-study. Lipids Health Dis. 2014 Oct 11;13:160. doi: 10.1186/1476-511X-13-160.
Bisht B. A multimodal intervention for patients with secondary progressive multiple sclerosis: feasibility and effect on fatigue. J Altern Complement Med. 2014 May;20(5):347-55
Pastore RL, Brooks JT, Carbone JW. Paleolithic nutrition improves plasma lipid concentrations of hypercholesterolemic adults to a greater extent than traditional heart-healthy dietary recommendations. Nutr Res. 2015 Jun;35(6):474-9.
Boraxbekk C J, Stomby A, Ryberg M, Lindahl B, Larsson C, Nyberg L, Olsson T, Diet-Induced Weight Loss Alters Functional Brain Responses during an Episodic Memory Task. Obes Facts 2015;8:261-272
Stomby A, Simonyte K, Mellberg C, et al. Diet-induced weight loss has chronic tissue-specific effects on glucocorticoid metabolism in overweight postmenopausal women.Int J Obes (Lond). 2015 May;39(5):814-9.
Manheimer, E.W., van Zuuren, E.J., Fedorowicz, Z., Pijl, H. Paleolithic nutrition for metabolic syndrome: systematic review and meta-analysis. Am J Clin Nutr. 2015;102:922–932.
Otten J, Mellberg C, Ryberg M, et al. Strong and persistent effect on liver fat with a Paleolithic diet during a two-year intervention. Int J Obes (Lond). 2016 Jan 20.
 stick to the facts here: I am extremely diligent about following a strict gluten-free diet. I do eat Amy’s products, and have for years.
stick to the facts here: I am extremely diligent about following a strict gluten-free diet. I do eat Amy’s products, and have for years.





 I love to bake. And I love to make candy. Not all the time, of course, because I’m sure it would get old quickly, but I typically make special treats a few times a year. For me, feeding people is my first language, and making desserts is one way of celebrating holidays and special occasions. I enjoy making desserts more than I enjoy eating them, actually, which is one of the first reasons why my husband and I connected. 😉
I love to bake. And I love to make candy. Not all the time, of course, because I’m sure it would get old quickly, but I typically make special treats a few times a year. For me, feeding people is my first language, and making desserts is one way of celebrating holidays and special occasions. I enjoy making desserts more than I enjoy eating them, actually, which is one of the first reasons why my husband and I connected. 😉
 absolute favorite!
absolute favorite!


















 *please note, some posts on this website do contain affiliate links*
*please note, some posts on this website do contain affiliate links* locally, and so does Roberta’s in Fairfax.
locally, and so does Roberta’s in Fairfax. April is IBS awareness month, and for way too many of my years, I’ve been entirely too aware of IBS. You could say it owned me for parts of the past decade. I know many of you can relate.
April is IBS awareness month, and for way too many of my years, I’ve been entirely too aware of IBS. You could say it owned me for parts of the past decade. I know many of you can relate. I’ve been blogging for 9 years now. 9 years! So, to celebrate, I give you fudge.
I’ve been blogging for 9 years now. 9 years! So, to celebrate, I give you fudge.

 Stumble It!
Stumble It!
